Common Types Of Moles And How To Tell When You Should Worry
It's the largest organ in the body. It protects us from toxins and pollutants. It shields us from all sorts of harm and hazards. It literally holds us together. Yet it's easy to take the body's unsung hero for granted.
It's your skin, the supple fortress that envelops and protects you from the outside world. But it's also more than that. Your skin is the map of your life and, often, a key index of your health. From scars and stretchmarks (yes, they happen to us all) to freckles and age spots (yup, they happen too), your skin charts the trajectory of your life.
And when you take a good look, you're likely to find that your skin is quite the shape-shifter, undergoing a lot of changes over the years. Among the most common of these changes is the appearance — and disappearance — of skin moles. Often, these changes are perfectly normal and entirely benign. But Sometimes, however, the emergence of new moles or a change in an existing mole's appearance can signal something more serious, including skin cancer. So what are the most common types of moles, and how do you know when you need to worry?
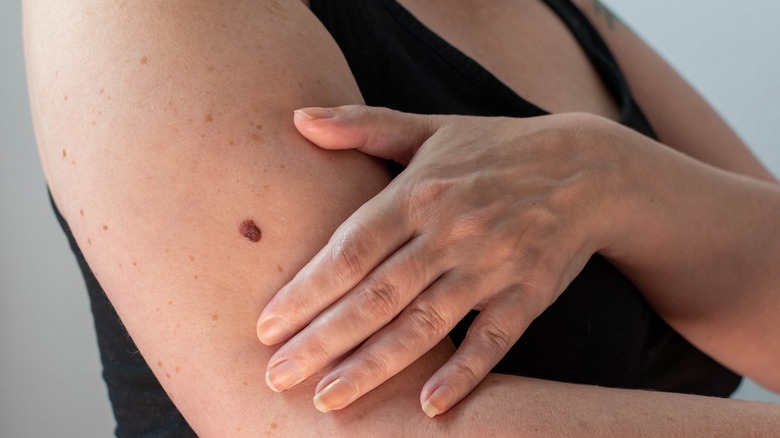
Acquired moles
Acquired moles refer to any mole that develops after birth. These are the most common types of moles, or nevi (plural for 'nevus'), and are usually harmless. The Cleveland Clinic notes that most people have anywhere from 10 to 40 skin moles. These often develop before the age of 30 and can range in color from pink to tan to dark brown or black. They may be flat or elevated, and they may have hair. Often, moles will change slightly over time, often becoming lighter and more elevated. Some will disappear.
However, if the mole is larger than the tip of a pencil eraser, has irregular borders or colors, or if it itches, bleeds, oozes, or hurts, then it should be checked by a doctor. Likewise, if you notice significant changes in a mole, or if you're over 30 and you find a new growth, it's wise to have it checked (per the Skin Cancer Foundation).
In addition, the Mayo Clinic urges that if you have an unusually high number of moles (i.e., more than 50 moles), you are at higher risk for skin cancer and will want to be especially conscious about skin protection and monitoring.
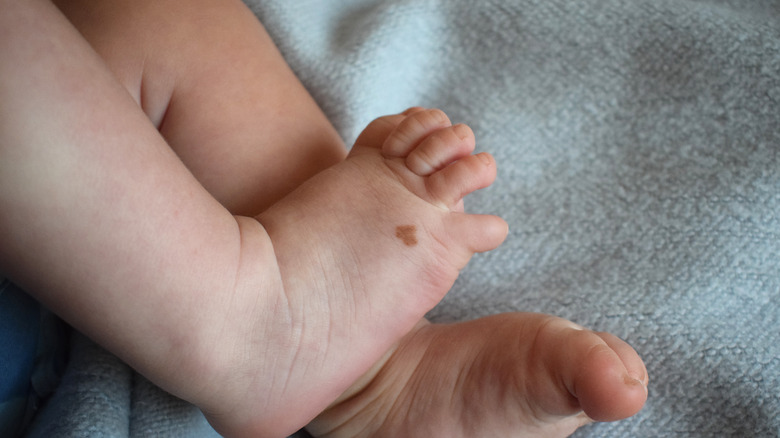
Congenital moles
While there are few things softer or more perfect than a baby's skin, it's not all that unusual for babies to be born with one or two skin moles. These congenital moles, also known as congenital nevi, are typically harmless. Some congenital nevi fade and even disappear over time. However, some nevi "grow proportional to the child's growth," according to the Children's Hospital of Philadelphia, which may put the little one at risk for physical or psychological impacts.
For instance, children with large congenital nevi may feel self-conscious, particularly if the growth is in a highly exposed area. They may also experience discomfort or impaired functioning if the mole is raised, which may cause it to become irritated or inflamed. There is also evidence that the larger the growth, or the greater the number of congenital nevi, the higher the child's risk of developing melanoma.
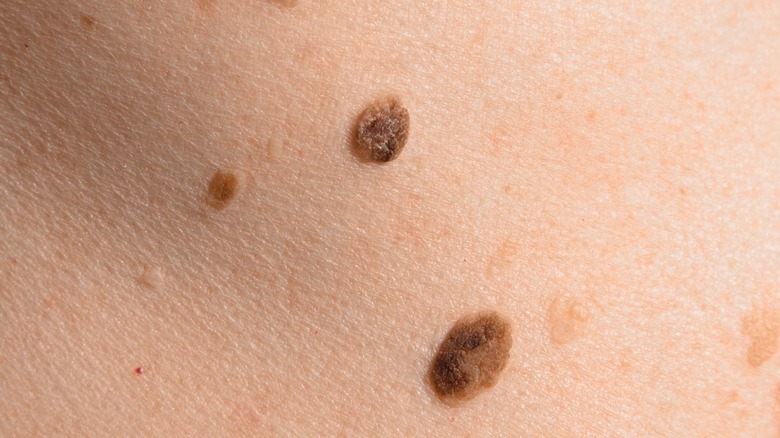
Atypical or dysplastic moles
Atypical or 'dysplastic' moles are ones that particularly bear watching due to their size and shape. These moles tend to be relatively large (i.e., bigger than a pencil eraser), have an irregular shape, and are varied in color. They're also often congenital and hereditary, so you may have been born with these atypical moles, and/or you might have immediate family members with a history of benign growths.
'Typical' moles generally have a uniform shape — often round — and their coloration is largely uniform as well, ranging from light brown to amber to a darker chocolate hue. Atypical moles, on the other hand, often show significant color variations, frequently appearing darker toward the center and fading out toward the edges. The borders, likewise, tend to be quite asymmetrical.
Atypical moles should be evaluated and monitored, especially if they appear suddenly or if they change in appearance. This is because, according to the Cancer Treatment Centers of America, though it's not common for dysplastic nevi to become malignant, it can happen. If you have more than five atypical moles, your risk of developing melanoma is estimated to be 10 times that of the general population (per the National Cancer Institute). And that makes vigilance, but not panic, the order of the day.
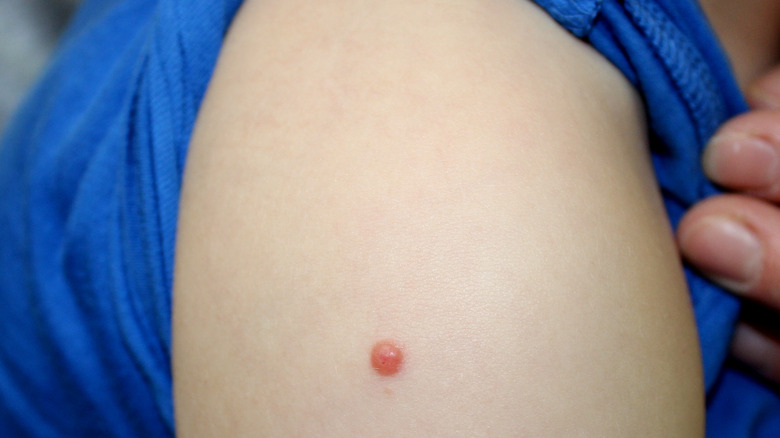
Spitz nevus
Another common type of mole can be significantly more difficult to identify correctly. They're called Spitz nevus, and they're usually harmless — but, let's face it, they can be pretty scary. That's because Spitz nevi often closely resemble melanoma.
In fact, they often look so much like melanoma that even your dermatologist may not be able to differentiate between them without a biopsy. According to Medical News Today, Spitz nevi usually develop before the age of 35, and they may ooze or bleed, which is why they may so easily be mistaken for malignant skin cancer. Unlike most typical moles, Spitz nevi are usually, but not always, pink and "dome-shaped."
Even though Spitz nevi are quite rare and are non-cancerous, it's important to have them promptly evaluated by a dermatologist. Their resemblance to melanoma in size, shape, color, and behaviors (i.e., large, irregular, and bleeding or oozing) means they're not something you want to play around with. Much better to be safe than sorry!
Pigmented lesions and age spots
Nevi, of course, are by no means the only kinds of changes you're likely to discover on your skin over time. Other localized changes are pretty common and, in most cases, aren't a cause for alarm. But, as with any deviation from your usual "norm," they bear watching.
Hyper-pigmentation, or localized dark spots on the skin, happen to us all. They're usually caused by sun exposure but are also often simply a normal aspect of aging, according to Oregon Health & Science University. That means that freckles and "age spots" aren't in themselves anything to be concerned about. But they should serve as a warning that perhaps you're not being as conscientious about sun protection as you should be. After all, there's no such thing as "good" sun damage. When your skin reacts to sun exposure, whether by freckling, tanning, or burning, that means harm has occurred. Yup, like the unicorn, a "good" tan simply doesn't exist.
Light-skinned people tend to be more prone to freckling and "age spots," especially if they have spent a lot of time unprotected in the sun. And both their fair complexion and their excessive sun exposure put them at elevated risk for skin cancer (per Cancer Research UK). So if you find that your skin is looking a bit more dappled than usual, it's a good idea to up your sun protection game, including integrating sun-protective clothing and makeup into your must-have wardrobe, no matter the season.
Knowing the warning signs
As scary as the thought of melanoma is, you're by no means powerless against it. Being a good skin steward is your most important weapon in the fight against skin cancer. This means ensuring that you're alert and aware.
Knowing what to look for when it comes to early skin cancer warning signs means that you'll be able to detect — and address — potential problems early before they can evolve into something severe. As reported by the American Cancer Society, the five-year "relative survival rate" for people with "localized" melanoma (i.e., melanoma that has not yet spread to other parts of the body) is around 99%. However, once the malignancy begins to spread, becoming a "regional" or "distant" growth, survival rates drop to 71% and 32%, respectively.
This is why it's so vital that you know the warning signs and that you make skin self-examination a routine part of your health regime, right alongside your monthly breast self-exam or your annual checkup and mammogram, and other preventative screenings.
When your moles hurt, itch, crust, ooze, or bleed
One of the first and most important warning signs to be on the lookout for is if you have a mole that crusts, itches, hurts, oozes, or bleeds. Typical nevi, those moles that are common and benign, should be pretty much unnoticeable. They may become more elevated over time, but they also generally lighten in appearance, becoming less obvious. That is certainly not the case with malignancies.
If a pre-existing mole begins to change, suddenly becoming inflamed, painful, itchy, bloody, or irritated, you should see a doctor promptly, according to the NHS. Likewise, if a new mole develops, especially if it has any of these concerning signs, you should promptly schedule an examination. Because these symptoms are common with melanoma, it's wise to err on the side of caution and attend to any potential problem quickly.
When you develop new moles
As we've seen, it's really common for new moles to develop or for freckles and sunspots to appear over time, especially if you spend a lot of time in the sun. However, most acquired moles form in childhood. As previously noted, acquired moles generally don't develop after the age of 30. This is why, if you are over 30 and you notice a new growth, the safest course is to have it evaluated. In fact, because most acquired moles develop in childhood, the Skin Cancer Foundation advises any adult who develops a new mole to see a dermatologist.
Likewise, if the new growth is larger than a pencil eraser, has irregular borders, is varied in color, or if it bleeds, oozes, crusts, itches, or hurts, it should be examined by a doctor, no matter your age. The American Academy of Dermatology recommends that patients use the "ABCDEs of melanoma" when monitoring new and existing skin growths: A for asymmetry, B for border, C for color, D for diameter, and E for evolving. When a mole looks concerning from any of these five perspectives, it's time to get it checked out.
Know your body
As vital as it is to remain alert to any relevant changes in your skin, you might not always recognize a red flag when you see it. Protecting against skin cancer means knowing your skin. And that means it might not be enough simply to eyeball it. The Skin Cancer Foundation notes that the more moles you have, or if you have moles larger in circumference than the eraser on a pencil, the more vulnerable you are to skin malignancy — so you'll want to be vigilant about each mole on your body.
If you want to do things right, then you're going to need records. Examine every inch of your skin, and take pictures and notes. And don't forget to check those often overlooked areas, such as your ears, your scalp, the backs of your legs, and even the soles of your feet. Any area of the body can develop skin cancer, whether it's exposed to the sun or not.
According to the American Cancer Society, you should do one of these self-exams regularly — ideally at least once a month. Use the previous month's notes and photos as a base for comparison. And remember that you're probably not going to be able to get a good view of every area, even with a mirror or camera, so ask your spouse to be your eyes for a while. And then return the favor — it can be a great way for partners to show one another a little bit of love!
Know your history
If you have skin, then you can get skin cancer. But that doesn't mean that everyone's equal risk. Complexion, of course, plays a significant role, as we've seen. If you're fair-skinned, then you're more vulnerable. Lifestyle, too, plays a key role. If you spend a lot of time unprotected in the sun, then you're likely accumulating sun damage that may evolve into skin cancer.
But family history also plays an important role. If you have multiple first or second-degree relatives (i.e., children, parents, siblings, grandparents, aunts, uncles, or nephews) with melanoma, then your risk of developing the disease may be up to 70 times greater than that of the general population, according to the AIM at Melanoma Foundation.
Likewise, if you have had a history of skin cancers, whether benign or malignant, then you're at risk for developing more in the future, per Cancer Research UK. This is why anyone with a personal or family history of skin cancer must be especially vigilant about sun protection, having regular dermatological exams, and monitoring their own skin with monthly self-checks.
Be a good skin steward
As with any health condition, there are some risk factors that are simply beyond your control. You can't do anything about your family history or turn back time and reduce your sun exposure. What you can do, though, is be a good skin steward today and for every day to come. You can create a lifestyle that protects the precious sheath that protects you.
Monitor your skin with thorough self-checks every month and see a dermatologist regularly, at least once a year, when everything is status quo and immediately when concerning changes arise. Above all, being a good skin steward means doing all you can to help your body stay healthy and strong. This includes guarding against sun damage by wearing sunscreen every day, even in winter or when it's cloudy outside. This is vital even if you have a darker skin tone or are a person of color.
The CDC recommends that people limit their sun exposure by avoiding both indoor and outdoor tanning and by staying out of the sun when "the UV index is 3 or higher." It's also important to choose the best sunscreen for your skin, and apply it generously throughout the day, even when you're just going about your daily routine, as even brief periods of sun exposure as you go about your day can cause significant damage over time. Hats and sun-protective clothing are also a great idea, as is an immune-boosting diet that consists of good sleep, regular exercise, and a nutritious diet.
Don't panic if you notice changes
Cancer is always scary. No one likes to think about it, let alone entertain it as a real possibility in their own life or the life of someone they love. And that's why sometimes it's easier just to ignore it, deny it, and go on about your day. When it comes to cancer, though, denial is by no means your friend.
And for cancers like melanoma, which are highly curable when caught early, any delay in treatment will just make the path to recovery longer and more difficult. So the smart and brave thing is to remain alert, aware, informed, and vigilant. But that doesn't mean, though, that when you notice a change, you should automatically assume it's cancer. The skin is a living, ever-evolving thing.
There are many reasons why a mole might change in appearance or suddenly become irritated when it wasn't before. There are also many reasons why new growths might suddenly appear. The key is to be calm, conscientious, and proactive. Learn all you can about your body and what it needs to remain healthy and strong. Understanding the real reason why moles suddenly appear, what causes new growths, and why an unexpected arrival on your skin is a cause for action (but not for panic) can help you on your journey to being proactive with each mole that appears on your skin.