Is Long-Form Birth Control Right For You? Everything You Need To Know
Despite what the current political climate might suggest, human beings have been using various forms of contraception to control their fertility for thousands of years. While the majority of these methods were rooted more in myth than scientific fact, and therefore likely wouldn't earn an FDA stamp of approval today, anthropological and historical evidence proves the human desire to control reproduction isn't anything new.
Post-modern, short-term contraceptives such as condoms, diaphragms, and "the Pill" have been effective and (mostly) readily available options for decades. The latter is still a popular choice today, with more than 151 million women worldwide taking the Pill. But the introduction of a variety of other types of birth control methods in more recent years, many of which are highly effective, "set it and forget it" type options, are beginning to replace the popularity of these traditional contraceptives. These long-form options, also known as long-acting reversible contraceptives (LARC), allow women the freedom to choose what type of birth control works best for their lifestyles.
The beauty of so many options is that you are in the driver's seat of your own reproductive health. But, if you've only ever taken the Pill, how do you know if making the switch to a long-form option is right for you? Are there side effects you can expect, or a transitionary period you should prepare for? Before speaking with your doctor, consider the different long-form birth control options you have and their various pros and cons.
A quick refresher on oral contraceptive make-up and use
At the time of its release in the late 1950s, the Pill was a revolutionary healthcare technology. It was the first medicine of its kind to truly provide protection against pregnancy and agency for women who craved control over their own bodies and futures. "I would argue that effective contraception was probably in the whole of the 20th century the most important change for women," NYU history professor Linda Gordon tells Allure. By eliminating reliance on men to provide and procure birth control, women were empowered in mass to take care of themselves. And, even with the introduction of other types of birth control methods, it continues to provide female autonomy desperately needed in post-Roe v. Wade America.
The Pill, which is a broad term for over 40 different brands and types of oral contraceptives, is a small tablet made up of different synthetic sex hormones. Some have combinations of estrogen and progestin, while others, referred to as POPs, contain only progestin. When taken daily, the Pill and these hormones trick the body into thinking it is pregnant by preventing ovulation. The addition of progestin also thickens cervical mucus, which makes it difficult for sperm to enter the uterus. Each pack of birth control pills ends with a placebo week and consists of pills that do not contain progestin and estrogen. During this time of the month, the body sheds its uterine lining, mimicking menstruation.
The benefits of oral contraceptives
When it was introduced to the public in 1957, the Pill's sole purpose was simply to prevent pregnancy. To this day, oral contraceptives are a safe and simple way to remain pregnancy-free. When taken exactly as prescribed, the Pill is 99% effective against pregnancy. Factoring in human error in the form of a forgotten pill or late prescription refill, the Pill is closer to 93% effective.
While preventing unwanted pregnancy is one of the main reasons women take oral contraceptives, more than 58% of users take them for reasons completely unrelated to pregnancy prevention. There are a number of benefits to taking the Pill that can help women live healthier and altogether better lives. Hormonal birth control is useful for regulating hormonal fluctuations that, when left unchecked, cause irregular menstrual cycles, heavy or irregular bleeding, PMS, and hormonal acne. By preventing ovulation, the Pill also reduces painful cramping experienced during your cycle.
Oral contraceptives are beneficial for women who suffer from conditions like endometriosis, migraines, and anemia caused by heavy menstrual bleeding. Some research suggests that taking the Pill may help some women with Polycystic Ovarian Syndrome or PCOS, a condition that affects one in 10 women and causes inflammation, acne, facial hair growth, and insulin resistance, as well. Furthermore, oral contraceptives are proven to prevent osteoporosis, as well as reduce your chance of developing uterine and ovarian cancers up to 20 years after you stop taking them.
Oral contraceptives are effective but not for everyone
Despite their numerous lifestyle benefits, safety, and efficacy, hormonal birth control pills aren't for everyone. They come with potential risks such as blood clots, heart attack, or stroke. The Pill might not be safe for you to take if you have a history of high blood pressure, high cholesterol, breast cancer, or diabetes. Some women experience unpleasant side effects as a result of taking the Pill, and while many of these side effects go away as the body adjusts to the medicine, others may experience long-term symptoms such as weight gain, spotting, decreased libido, depression, and anxiety.
In recent years, a shift towards natural wellness largely sparked by social media influencers has put hormonal birth control pills and their side effects under scrutiny. While these side effects are possible and give many women considering their birth control options pause, many medical practitioners caution against quitting cold turkey just because a wellness influencer says to — especially with the current tenuous access to abortion care. "Everyone has a different risk-benefit ratio," ob-gyn Dr. Jen Gunter tells The Cut. "...Definitely if you're having depression, you should talk with your provider about whether contraception could be part of the picture. But it's also important to remember that if you are at risk of getting pregnant, what's going to be the plan? Because an accidental pregnancy is also not going to be good for your depression."
What exactly is long-acting reversible contraception?
If you are questioning your hormonal birth control pill or simply want something more permanent than a condom or diaphragm, long-acting reversible contraception may be the way to go. LARCs consist of a variety of birth control methods that are safe for long-term use, with certain contraceptives lasting for up to 10 years. Depending on the method you choose, LARCs are also 20 times more effective than taking the Pill.
LARCs are inserted or implanted in the body and come in both hormonal and nonhormonal options. Like most birth control methods, they do not protect against sexually transmitted diseases and they cannot cure diagnosed medical conditions, although they may ease or reduce certain symptoms like painful cramps or irregular bleeding. LARCs are often labeled as "permanent" birth control solutions, but they need to be replaced on a semi-regular basis to maintain their effectiveness. They are easily removed by a medical professional whenever you want. This doesn't affect your fertility, even if it isn't time to replace your device. Because of this, LARCs are perfect if you think or know you will want to become pregnant in the future, but don't want the hassle of daily or single-use birth control options.
IUDs
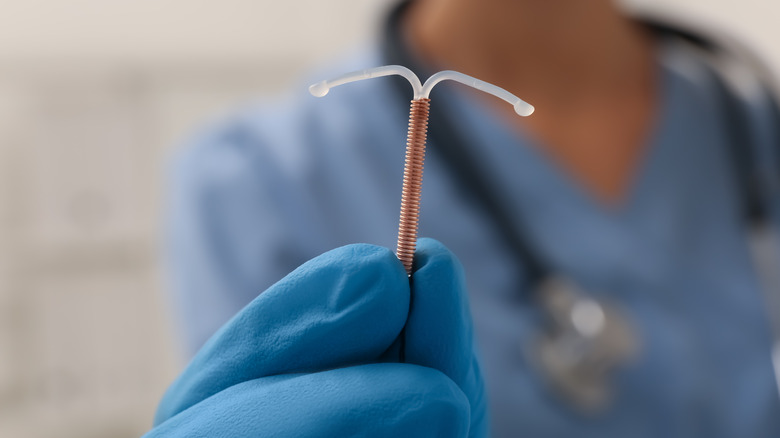
Intrauterine devices, or IUDs, are low-maintenance LARCs that are 99% effective in preventing pregnancy. These flexible, T-shaped plastic devices are inserted into the uterus by a medical professional during a pelvic exam, where they sit snugly. IUDs are not visible when correctly placed, but they do have thin plastic strings attached to the end which hang an inch or so out of the cervix. These strings are used by your doctor to pull the IUD out when it is time to replace or remove the IUD.
The insertion process for IUDs ranges from mild discomfort to pretty painful, and it is usually recommended that patients take an over-the-counter painkiller like Advil an hour before the procedure to help with the cramping. Once inserted, IUDs work locally, preventing pregnancy from within the uterus itself. You don't have to think about it again until it's time to replace it. Currently, there are five IUD options available to choose from, including four hormonal and one non-hormonal.
"IUDs are a safe and highly effective birth control option for most people of all ages — from young people who had not had children to people in their 50s who haven't yet hit menopause," Dr. Gillian Dean shares with Elle. "It's safe to get an IUD even if you've never had penetrative vaginal sex. Your sexual history shouldn't impact the method of birth control you decide to use."
What's the difference between copper and hormonal IUDs?
Skyla, Liletta, Kyleena, and Mirena are the four hormonal IUD brands approved for use in the U.S. All hormonal IUDs contain different amounts of the synthetic hormone progestin and last for anywhere from three to eight years. Like birth control pills, the release of progestin thickens cervical mucus and prevents sperm from getting through to the uterus. It also stops ovulation. As a result of these functions, many women experience lighter bleeding and reduced cramps while using hormonal IUDs, while some stop getting their periods altogether.
Paragard, the copper IUD, is the nonhormonal IUD option. With Paragard, you will ovulate as normal. However, the thin coil of copper wire wrapped around the IUD causes an inflammatory reaction within the uterus that makes it an inhospitable environment for sperm. Copper IUDs can remain in place for 10 years, and while they may temporarily increase cramping and bleeding, they do not have the risk of more serious side effects like blood clots that hormonal birth control carries.
That being said, both copper and hormonal IUDs come with certain risks you should be knowledgeable of before making the switch. "Anytime you insert the IUD, whether it be copper or hormonal, there's always a risk of bleeding and infection," Dr. Tamika K. Cross tells Cosmopolitan. Though rare, there is also a risk that IUDs may poke a hole in the uterus and embed themselves in the uterine wall, which may require surgery to remedy.
Hormonal implant
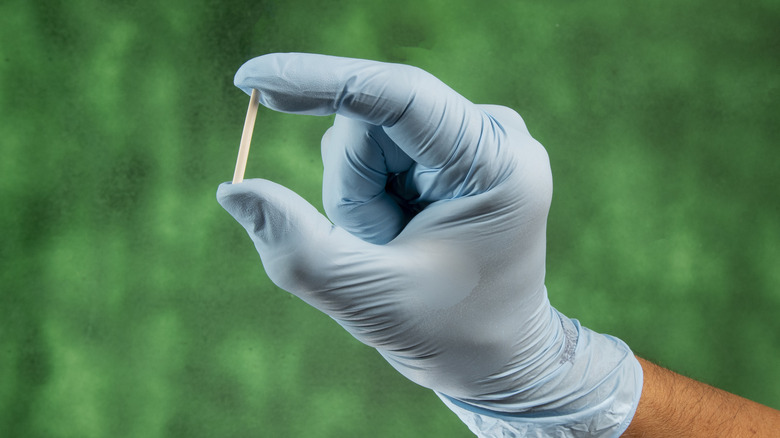
If an IUD doesn't sound like your style, the hormonal implant Nexplanon is another long-term birth control option worth considering. The hormonal implant is a matchstick-sized rod that is inserted under the skin of the upper arm by your doctor. It contains progestin which is released in a steady, small dose for three years. Like IUDs, the hormonal implant is a set-it-and-forget-it type of contraception that is 99% effective in preventing pregnancy for the duration of its life.
The insertion procedure is considerably less painful than the IUD and only takes a few minutes. After conducting a urine test to confirm you aren't pregnant, your doctor will apply a local anesthetic to the area of your arm where the implant will be inserted. Usually, it is placed on the inner arm of your non-dominant hand. Then, your doctor will apply the preloaded insertion device to the numb area and insert the plastic rod until it is secured in the layer of fat beneath the skin. This procedure may cause some bruising or short-term tenderness at the injection site.
The hormonal implant takes seven days to fully protect against pregnancy, which means you may need to use condoms or continue taking the Pill in the interim. This type of birth control cannot be used as emergency contraception, but it can be safely inserted right after giving birth or having an abortion.
Contraceptive injections
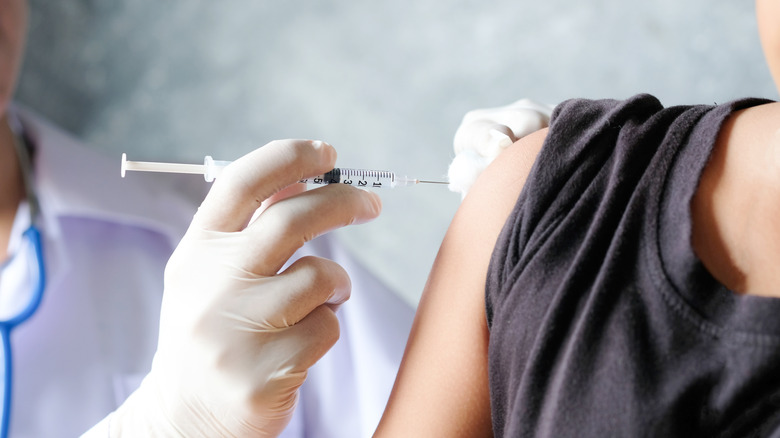
The Depo-Provera injection is a highly effective and more convenient form of contraception than condoms or the Pill. Also known as the depo shot, this form of birth control requires visiting your doctor every three months to receive an injection in the muscle of your arm or buttocks. It releases the hormone progestin to prevent pregnancy for up to 12 weeks and therefore contains the same risks and potential side effects as similar hormonal contraceptives. The depo shot can also contribute to bone thinning, a side effect that goes away if you discontinue use.
Many women prefer the depo shot over other types of birth control due to its discrete nature. Like long-form birth control options, the depo shot allows for spontaneity with your partner and interruption-free sex. It is also sought after for its ability to lighten or stop periods, a side effect that normally occurs after a year of receiving the shot.
Vaginal ring
While not technically an LARC, vaginal rings are an alternative birth control method for women who want more control over their own sex lives and fertility. The vaginal ring, sold under the names NuvaRing and Annovera, is a small, flexible ring placed inside the vagina. The ring stays in place for three weeks and is taken out for one week. You are still protected against pregnancy for the week the ring is out, although a new ring must be inserted when the week is up to maintain 24/7 protection. You can also safely skip periods with the vaginal ring if you choose, a major benefit its users tend to appreciate. It requires a prescription from your doctor to obtain but can be safely inserted in the comfort of your own home.
The vaginal ring protects against pregnancy for one month by releasing a steady stream of estrogen and progestin into the vaginal lining. Together, these hormones halt ovulation, thicken cervical mucus, and thin the lining of the womb, making it harder for a fertilized egg to implant.
The birth control patch
The birth control patch is another form of hormonal birth control more reliable than the Pill or condoms but less invasive than a long-form method like IUDs or implants. Instead, this contraceptive method releases estrogen and progestin via a square adhesive patch applied to the skin. The patch is worn on a daily basis for three weeks and can be placed on the stomach, upper arm, buttocks, or upper back. During the fourth week, the patch is removed and a normal period commences.
When used correctly, the patch is 99% effective. This number decreases if you forget to apply the patch or if you take certain antibiotics, antifungal medications, or seizure medications. The patch also has a weight limit. If you weigh more than 198 pounds, the patch may not work appropriately. Common side effects with the patch include bloating, irregular bleeding, moderate weight gain, nausea, skin irritation, and yeast infections. It is also unsafe for women who smoke or have a history of blood clots, stroke, breast or uterine cancer, or diabetes. On the other hand, the patch has numerous benefits including preventing breast and ovarian cysts, reducing cramping, reducing hormonal acne, and giving users lighter periods.
Long-form birth control ultimately allows for more control over your fertility
The importance of all forms of birth control, as well as its availability to women around the country, cannot be denied. As Dr. Jerilynn Prior tells Bustle, "We now not only have the power to control our own reproduction — but also to affirm our own natural physiology." However, it is just a fact that some contraceptive methods work better for certain people than others. While some women don't mind condoms or a daily pill, others prefer the worry-free reliability and effectiveness of a long-term option.
Ultimately, you are the only person who can decide which form of short or long-form birth control is right for you. "I always just say that the best contraception is the one that works for you," Dr. Stacy De-Lin, gynecologist and associate medical director of Planned Parenthood of Southwest and Central Florida shares with SELF. "It's the one that you like, the one that you appreciate using and doesn't cause you any issues."