Um, Is Allergy Medication Messing With Our Skin? Here's What To Know
Allergy season is not a great time for any of us. Most of us find ourselves having to take some form of medication until the allergies pass, but have you ever considered that there may be certain side effects your medicine might be causing? One such effect is that it could give you skin problems.
According to the Mayo Clinic, some popular antihistamines include Cetirizine (Zyrtec, Zyrtec Allergy), Desloratadine (Clarinex), Fexofenadine (Allegra, Allegra Allergy), Levocetirizine (Xyzal, Xyzal Allergy) and Loratadine (Alavert, Claritin). These aren't all of them, of course, but if any of them sound familiar to you or if you are prescribed any of them due to allergies, it might be worth noting that they could be affecting your skin condition. It's important to educate yourself on exactly how these medications could interact with your body so you can take preventative measures to make sure your skincare is intact.
How do they work?
Here is how the National Health Service, one of the most reputed healthcare services in the world, explains how antihistamines primarily work. They note that "antihistamines block the effects of a substance called histamine in your body." Histamine is what helps to attack infections by making your blood vessels expand. This is also why your skin swells when you're having an allergic reaction. They explain that "in people with allergies, the body mistakes something harmless — such as pollen, animal hair or house dust — for a threat and produces histamine." This is why taking antihistamines can help you prevent experiencing allergic symptoms.
However, antihistamines also have certain side effects, as do the majority of medications. The NHS notes that some of the most notable side effects are sleepiness, dry mouth, blurred vision, and difficulty passing urine. Another less talked about side effect is some of the implications antihistamines can have on your skin with long-term use.
Dry skin
William Reisacher, director of allergy services at Weill Cornell Medicine and New York-Presbyterian, told Allure that "because of their effects on the oil production for the skin, long-term use can lead to dry, itchy skin," noting that "there are histamine receptors on cells of the skin that stimulate them to release sebum, or oil, onto the skin." As antihistamines work by blocking histamines, they can affect your skin's sebum production, resulting in dry skin.
Reisacher also emphasizes that long-term use of antihistamines "can also produce dryness in the nose and throat region, causing post-nasal drip and nosebleeds," so it is not recommended that you use antihistamines for their skin drying capabilities if you have oilier skin either. However, Dr. Arash Akhavan, also a qualified dermatologist, explained to L'Oréal that "there is likely a negligible to the minor effect of antihistamines on sebum production" and that it's more affected by hormones.
Combating dry skin
The obvious antidote if you have dry skin is, of course, hydration. Especially if you're on antihistamines and have to take them long-term, dry skin is a concern you must address. But how does one hydrate their skin beyond obvious means, like drinking more water? According to the American Academy of Dermatology Association, there are a range of simple solutions that you can look to for combating dry skin.
They recommend that you "use warm rather than hot water" when taking a bath or a shower, and moisturizing your skin with a lotion immediately after your shower. They also note that certain ingredients will benefit you more than others to combat dry skin and hydrate it; some ingredients that the AADA recommends you look for in your hydrating products include dimethicone, glycerin, hyaluronic acid, lactic acid, lanolin, petrolatum, shea butter, and oils like jojoba oil and mineral oil.
Perioral dermatitis
Additionally, Dr. Teo Soleymani, a board-certified dermatologist from California, who spoke to Today, says that allergy meds can also cause "a flare of perioral dermatitis," noting, "When allergies are worse, and patients' asthma is worse, we do see an increase in perioral dermatitis related to inhaled steroids as well, especially nasal sprays."
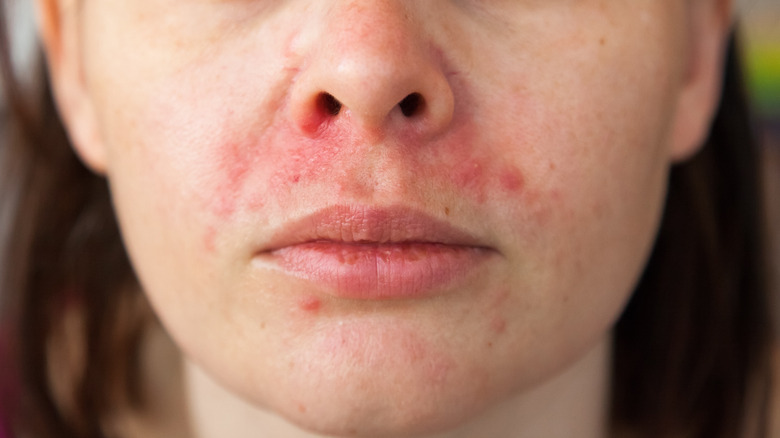
Perioral dermatitis appears as a rash on the face, near the nose and mouth, and Dr. Soleymani further explained that the condition can often be confused with an "eczema-like rash or contact dermatitis, but it actually falls in the acne and rosacea family." He says perioral dermatitis behaves very similarly to these other skin conditions. Along with bumps, you make notice a burning sensation on the lower half of your face, according to Mount Sinai. If any of these symptoms sound familiar to you during your allergy medication intake, you could potentially be suffering from perioral dermatitis.
When to see a doctor
If you start to experience a rash, it's always a good idea to consult a medical professional. Of course, it's not a cause for too much concern because treatment options for the condition are plenty. According to Cleveland Clinic, a nonprofit American academic medical center, your doctor can normally diagnose perioral dermatitis just by looking at your skin. However, a skin biopsy is also an option in some cases.
They note that it is a good idea to stop using your steroids, like your antihistamine, if you have perioral dermatitis. You should also avoid using topical creams for your face, including makeup and your moisturizer. Fluoridated toothpaste and gum is also not great.
Health professionals at Cleveland Clinic say that when you make an appointment with your dermatologist to treat your condition, they will most likely prescribe topical medications such as pimecrolimus, azelaic acid, tacrolimus ointment, and adapalene. You might also be given oral medications such as tetracycline, doxycycline, or minocycline. Please keep in mind that although it is good to be in the know of what to expect from your prescription, you must never take any of these medications without consulting a medical professional first.