What To Know Before Getting Your First Mammogram
Breast cancer is an anxiety-inducing topic for many. It is a relatively common type of cancer that can occur in both men and women, although it is much more common for women to be diagnosed. According to the CDC, approximately 1 in 8 women in the United States will get breast cancer during their lifetime. It is the second-leading cause of cancer deaths among women with over four million current diagnoses throughout the country (via Mayo Clinic). This may sound overwhelming, but there is good news. Increased funding for breast cancer research, as well as greater awareness surrounding early detection, are helping increase survival rates and decrease the prevalence of the disease.
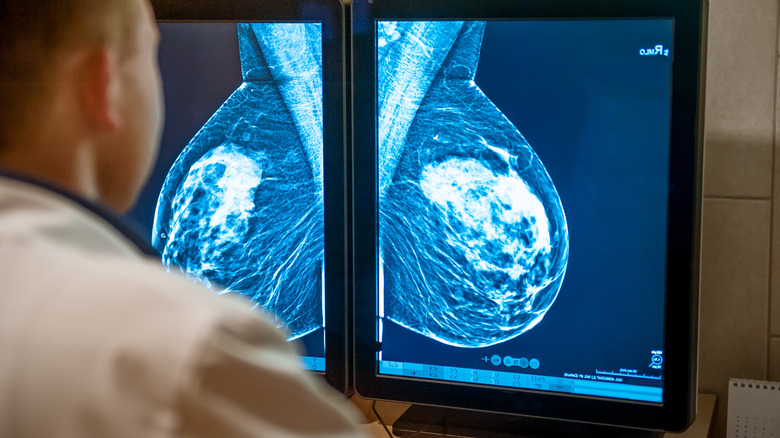
Currently, mammography screenings are the best way to identify breast cancer in its early stages. A mammogram, which is a low-dose X-ray picture of the breast tissue, allows medical professionals the ability to find instances of cancer up to three years before it presents physical symptoms. According to BC Cancer, identifying breast cancer early is imperative to help women receive access to a broader range of treatment options and increase their chance of recovery. Furthermore, regular screenings are proven to reduce breast cancer deaths by more than 25%.
Despite their effectiveness and monumental importance, getting a mammogram for the first time can be a nerve-racking experience. Here's everything you need to know about getting your first mammogram, including how to prepare the night before, what an actual mammogram is like, and what happens after you receive one.
When should you get your first mammogram?
You may already know the importance of getting a mammogram, but knowing when to get your first one can be a bit confusing. Generally speaking, you should get your first mammogram between 40 to 44 years old. Although breast cancer is more commonly experienced by women ages 65 to 74, establishing a baseline reading helps identify issues down the line (via U Health). After your first mammogram, you should plan to schedule an annual mammogram until you reach the age of 54, per Samaritan Health Services. Once you reach that age, it is normal to have a mammogram once every two years.
This rule does not apply to women who are at a higher risk of developing breast cancer. Having a family history of breast cancer, a personal history of breast cancer, as well as the presence of certain genes, can increase a woman's risk of developing breast cancer during her lifetime, according to Susan G. Komen. It is normally recommended that women with these risk factors begin getting regular mammograms starting around age 30 or 35. However, unless you and your doctor have discussed the need for one, getting a mammogram earlier than age 40 is usually unnecessary.
When to schedule your first mammogram
Believe it or not, there are better times to schedule a mammogram than others. According to a 2009 study by Dr. Diana Miglioretti, premenopausal women benefit from scheduling their mammogram during the first week of their menstrual cycle (via ScienceDaily). During this time, the breast tissue is less dense, which makes it significantly easier for the x-ray unit and radiologist to pick up any abnormalities.
As a bonus, breasts are typically less tender or sensitive during the beginning of the menstrual cycle, according to Fred Hutch Cancer Center. Due to the nature of a mammogram procedure, scheduling your first mammogram before your period can eliminate a lot of physical discomfort. Of course, many women cannot accurately track or predict their menstrual cycle. It can be difficult to track it for normal life purposes, let alone to be able to schedule doctor's appointments around it. However, research published in the journal, Radiology, notes that scheduling your first mammogram around your period has not been clinically proven to affect specificity or cancer detection rate (via National Library of Medicine).
You should avoid scheduling your first mammogram if you are pregnant or breastfeeding. If you aren't sure, talk to your doctor before scheduling the exam.
How to prepare the night before a mammogram
Many medical procedures require special preparation the night before. However, mammograms require very little. You don't need to take pain medicine, although over-the-counter (OTC) meds like Motrin, Aleve, or Tylenol are okay if you're worried about experiencing pain during the procedure, according to Healthline. It is also important to continue taking any daily medications prescribed by your doctor unless specifically instructed not to (via Hackensack Meridian Health). And it is fine to exercise as you normally would.
Fasting the night before a mammogram is not necessary. However, if you notice any particular foods, such as caffeine-heavy beverages or chocolate, increase breast tenderness, you may want to avoid them the night before your first mammogram. Research published in the Journal of Primary Health Care suggests that a high-fat meal before a mammogram may also contribute to breast tenderness that a mammogram can exacerbate (via National Library of Medicine). Despite this, most medical professionals agree that you can eat and drink as you normally would the night before a mammogram as these foods will not affect your test results.
Are beauty products and deodorant okay to wear during a mammogram?
According to Envision Radiology, you should refrain from using any personal care products on or near the breasts on the day of your mammogram. This includes deodorant, lotions, creams, perfume, powder, makeup, or antiperspirants. Products like these can show up as white areas or tiny, sand-like spots on the mammogram images, even if they are applied to areas like the armpits. Deodorants in particular, most of which contain aluminum or metallic substances, can appear as calcifications on the X-ray images (via BreastCancer.org). These specks can read as cysts, fatty cells, and cancerous or abnormal tissue, thereby affecting your test results. This can then lead to further unnecessary testing or repeat imaging procedures. It's okay if you forget. Simply let the tech know before the procedure and they will provide you with wet wipes to remove the product (via Pure Mammography).
It is recommended that women schedule their mammograms early in the day, especially if going without personal care products like deodorant makes them uncomfortable. Alternatively, you can bring your items with you and put them on after your mammogram. Some women are also concerned or embarrassed about exposing their tech to body odor. While this anxiety is understandable, remember that radiologic technologists are healthcare professionals who perform mammograms day in and day out. They're unlikely to notice or comment on it. Their goal is to make you feel as comfortable as possible to get the images they need.
What type of clothing should you wear for your first mammogram?
Believe it or not, the type of clothing you wear during your first mammogram is also important. The clothing items themselves won't affect your test results, so technically you can wear whatever you want. However, certain items aren't exactly conducive to a comfortable procedure on your end.
During a mammogram, you will need to remove all of your clothing from the waist up. This means that one-piece items like a dress, romper, or jumpsuit aren't ideal. If possible, choose a loose, two-piece outfit that will allow you to easily remove the top half but keep your bottom half covered, per Maiden Lane Medical. You will be provided with a hospital gown that opens from the front to wear during the mammogram (via Marshall Medical Centers). It is also recommended that you avoid wearing jewelry such as earrings, necklaces, or piercings. If you do wear jewelry to your appointment, it will most likely have to be removed before the procedure.
Things you should tell your mammographer
Communicating with your mammographer is important before and during the procedure. As the person who lives in your body, you are its expert. According to the National Breast Cancer Foundation, Inc., you should know what "normal" looks and feels like for your body. This means being aware of any physical changes or new abnormalities in your breasts. Changes might include how the nipples look, nipple discharge that is clear or bloody, lumps in the breast, or a change in skin texture. If you are considered at high risk of developing breast cancer, you should discuss those risk factors with your mammographer. Also, bring up genetic mutations associated with breast cancer such as the BRCA1 or BRCA2 genes, and your family history.
It is also important to share any hormones you're taking or previous surgeries in or near the chest area. If you have breast implants you need to tell your mammographer that as well (via Cancer.Net). Both silicone and saline implants generally make it harder for mammographers to see the breast tissue being imaged. Having implants does not exclude you from receiving a mammogram, it will just require additional images to help doctors get a fuller picture of the breast tissue.
During the mammogram, you should also feel free to talk to your mammographer about any pain or discomfort you are experiencing. Some pain is normal but it generally only lasts a couple of seconds. Extreme pain should be communicated to the mammographer immediately.
What does a mammogram entail?
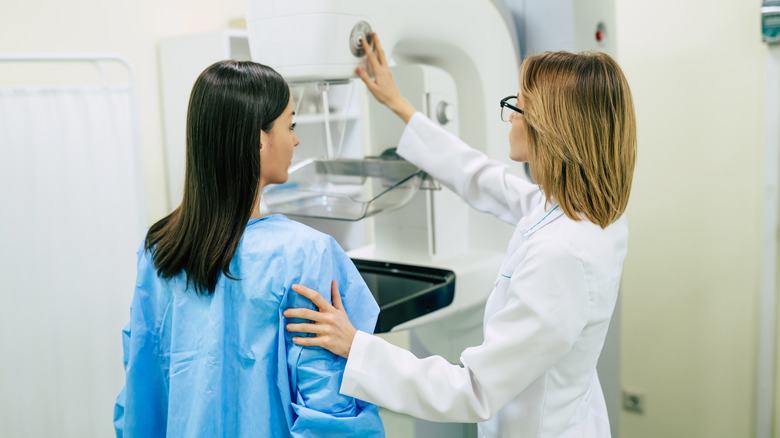
Now that you know how to prepare for a mammogram let's talk about what the procedure actually entails. According to RadiologyInfo.org, a mammogram is an outpatient procedure that uses a small dose of ionizing radiation to produce pictures of the insides of the breasts. The mammography equipment looks like a large box with a tube, which is what produces the x-ray images. It features a platform to rest the breast on and a plastic paddle that compresses the breast.
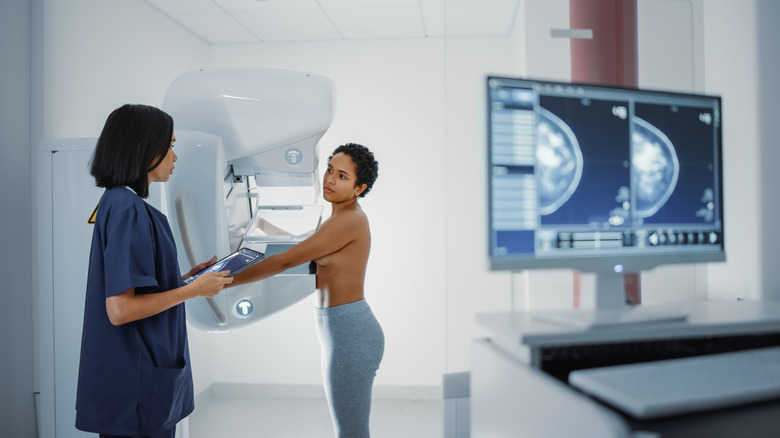
During the procedure, you stand in front of the unit with your breast on the platform (via CDC). The mammogram unit compresses the breast to even out the breast thickness and help make the tissue more visible. It also thins the breast, which allows for a lower dose of radiation to get an accurate image, and minimizes movement that can alter the image quality. You may be asked to hold your breath to help reduce movement as the pictures are taken. The X-ray technician will likely place stickers on prominent scars, birthmarks, and nipples to avoid confusion for the radiologist looking at the images later.
During a mammogram, you may be asked to move around to obtain the images the mammographer needs. A mammographer typically takes a top-to-bottom view and a side-angled view. Overall, most mammograms take between 20 to 30 minutes to complete. It is generally described as an uncomfortable procedure, although it only takes a few moments on each side.
Know what kind of mammogram you are getting
There are several different types of mammograms, and it is important to know which you are getting before your first appointment. According to BreastCancer.org, there are two main types: 2D digital mammograms and 3D mammograms, which are also referred to as digital tomosynthesis. The technique for each procedure is the same. However, the types of images they produce are drastically different.
A 2D digital mammogram creates a 2D image of the breast. This is the most common form of digital mammography and includes the standard top and side angle images (via Fox Chase Cancer Center). 3D mammograms on the other hand take multiple images of each breast. These images are then compiled in a computer to paint a complete picture of the breast.
Currently, not all hospitals have access to a 3D mammography unit. However, this cutting-edge screening technology not only helps reduce the rate of false positives and repeat imaging procedures but can find more cancers than its 2D counterpart. It is also easier to identify abnormalities in women with dense breast tissue. Neither is more recommended than the other by medical professionals. What is more important to major organizations such as the American Cancer Society is that women take part in the annual screenings in the first place.
Where can you get a mammogram?
There are numerous places you can get a mammogram outside of a normal physician's office. According to Know Your Girls, in addition to dedicated mammography clinics, you can get a mammogram at your local hospital or a radiology or imaging center. Many cancer centers also own mobile mammography vans. These mobile imaging centers are normally equipped with 3D mammography equipment and can travel from workplaces to rural areas to provide screening mammograms for women who might otherwise not have access.
If you aren't sure where to go for information on providers near you, consider finding a mammography provider by contacting the National Cancer Institute at 1-800-4-CANCER. They will be able to connect you with providers in your area that offer mammograms and other types of imaging procedures you may need. No matter where you get your mammogram, make sure to choose a facility accredited by the American College of Radiology (ACR) that has a reputation for high-quality equipment and experienced staff (via BreastCancer.org).
Are mammograms painful?
Many women who have never had a mammogram before are worried that the procedure will be painful. After all, in order to achieve the right kind of images, each breast must be compressed with a paddle or two acrylic plates. According to Beaumont, although general discomfort is likely, experiencing actual pain isn't. Individual pain tolerance will play a role, however, most women find they can tolerate the discomfort easily. Receiving the actual X-ray is painless.
Women with larger breasts are often concerned that the compression required to flatten their breasts appropriately will cause significant pain. According to Sharp, breast size is extremely unlikely to play a role in either pain or image quality during a mammogram. Other factors may affect your sensitivity to a mammogram, however. The skill of your technician, the actual shape of your breasts, and your positioning during the exam can potentially lead to an increase in discomfort. Remember to tell your X-ray tech if you experience any sharp or intense pain during the exam.
Minor bruising is not uncommon in the days following a mammogram, especially for women who take blood thinners (via Healthline). It might be more comfortable to avoid underwire bras after your first mammogram as well.
What is dense breast tissue and will it affect a mammogram?
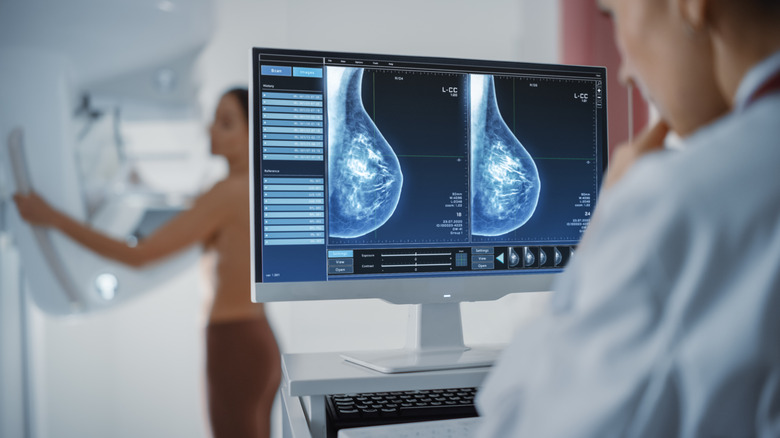
According to the National Breast Cancer Foundation, Inc., every woman's breasts are a mixture of fatty and fibroglandular tissue. Dense breast tissue has more fibroglandular tissue than a breast with more fatty tissue. It is not bad or uncommon to have dense breast tissue. Roughly 50% of women 40 and older have dense breasts, per the National Cancer Institute. It can be inherited or the result of a low BMI, although it isn't something you can feel during a self-exam. It is only possible to find out if you have dense breast tissue during a mammogram.
Having dense breast tissue can have an effect on mammogram images. This is because dense breast tissue shows up as white and opaque on the final images whereas fatty tissue appears dark and transparent. Mammograms of breasts with more dense tissue can be harder for radiologists to decipher because they can't see through it. Cysts, calcifications, and tumors also can appear as white areas on a mammogram.
Currently, the United States Preventive Services Task Force does not recommend additional imaging tests for women with dense breasts. However, it is important to note that having dense breasts are a risk factor for breast cancer. This risk is not associated with difficult imaging during a mammogram. Once you know you have dense breasts, you may want to ask your doctor about recommendations for additional testing or your individual risk.
What happens after a mammogram?
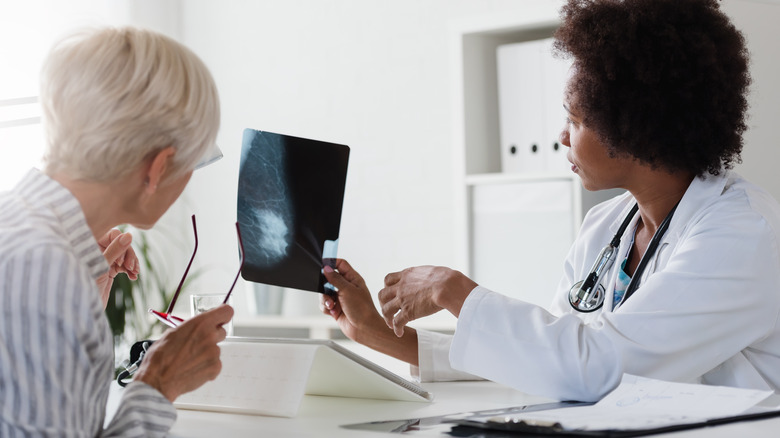
You will likely receive the results of your mammogram in two weeks or less (via Know Your Girls). This time frame is not set in stone, so it's best to ask your care team about when to expect the results. That way if you don't hear back from your doctor's office in the declared timeframe you can follow up.
If your mammogram shows areas of concern such as a lump or other abnormalities, your doctor will order additional tests. In the U.S., approximately 10-12 percent of women are called back after a mammogram for more tests, according to Know Your Girls. You may have to schedule an MRI or an ultrasound of the specific area to confirm it is non-cancerous. These additional tests may also need to be accompanied by a breast biopsy.
According to Mayo Clinic, breast biopsies involve removing a sample of breast tissue and sending it to a pathology lab for analysis. Breast biopsies are scary to think about, but 80% of women who receive them are not diagnosed with breast cancer. In fact, most abnormalities that require additional testing are not breast cancer, but rather benign conditions (via Susan G. Komen). However, if the results of your test indicate you do have cancer, your doctor will sit down with you right away to discuss treatment options.