Everything You Need To Know Before You Get Top Surgery
Many trans men and non-binary people experience chest dysphoria. According to the American Academy of Pediatrics, chest dysphoria is defined as "physical and emotional discomfort and distress caused by the presence of unwanted breast development." One study published in the Journal of Adolescent Health found that chest dysphoria was highly correlated with depression and anxiety, indicating the condition is a source of poor mental health for trans men and non-binary folks (via ScienceDirect).
People who experience chest dysphoria often undergo a procedure called top surgery, per the Mayo Clinic. During this procedure, a specialized plastic surgeon removes the unwanted breast tissue and shapes the chest to give it a more masculine appearance. Top surgery enables trans men and non-binary people to live in a body that reflects their gender instead of a body that reflects their biological sex. For many, top surgery relieves not only chest dysphoria but also a lot of gender dysphoria — the physical and emotional distress they experience because their gender assigned at birth doesn't match their authentic gender.
Top surgery is a complex procedure that requires a lot of preparation and recovery time. Here's everything you need to know as you consider and prepare for this life-changing surgery.
Surgical techniques for top surgery
The top surgery technique used varies depending on the body size of the patient, the amount of breast tissue, and the elasticity of the patient's skin, according to the University of California, Santa Barbara. The most common techniques used by top surgeons are keyhole, periareolar, inverted-T or "T Anchor," and double incision.
Thinner patients with smaller breasts are good candidates for the keyhole and periareolar techniques. For the keyhole technique, the surgeon makes a half-circle incision under the nipple and removes breast tissue through that incision. The periareolar technique is a bit more invasive as the incision circles the entire nipple. These techniques are the least invasive, create minimal scarring, and typically ensure that the nipples maintain sensation. However, they're not appropriate for patients with larger bodies or larger breasts.
The inverted-T or "T Anchor" technique is used for patients who want to maintain nipple sensation. It's the most invasive kind of top surgery because two incisions are made on each breast — one horizontal incision under the breast and one vertical incision from below the nipple to the horizontal incision.
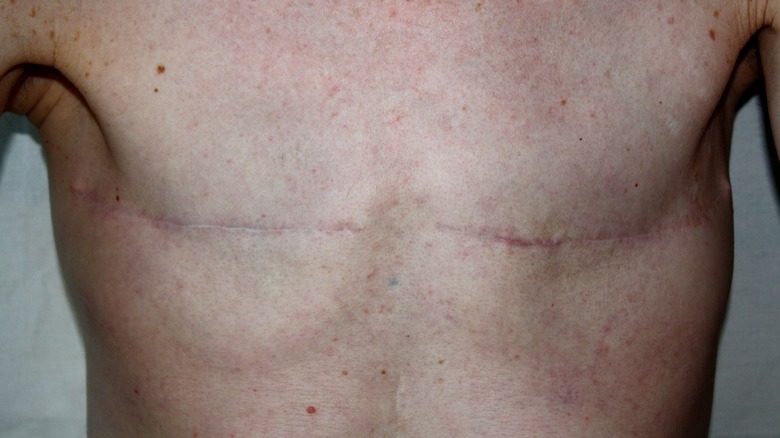
Aesthetically, the best top surgery results are achieved through the double incision technique, which involves two horizontal incisions under the breasts. Though this technique often results in the most masculine-looking chest, it's harder to preserve nipple sensations because the nipples are removed and replaced during the procedure. The double incision technique is appropriate for people of all sizes with medium to large breasts.
Potential risks of top surgery
It's important to understand that top surgery is a major surgical procedure, so it does have some big risks. According to the University of California San Francisco's Transgender Care program, serious complications from top surgery are rare.
About 5% of patients have extra skin after surgery which can make it difficult for the incisions to heal. Between 1 and 2% of people will develop hematomas, a buildup of blood under the skin that causes swelling. Certain trans folks are more prone to developing hematomas, so be sure to discuss this potential complication with your surgeon. Oil-filled cysts called seromas can also form in rare cases. Post-surgical infections are actually rare in top-surgery patients. The most common infection is cellulitis, which can be easily treated with antibiotics.
Aesthetic issues are the most common risks associated with top surgery. Some people aren't satisfied with the way their chests or nipples look after surgery. This can be due to issues with the nipple reattachment or graft, excess skin flaps, often called dog ears, or an imbalance in the amount of tissue remaining that becomes apparent during the healing process. Most of these issues can be corrected with follow-up outpatient surgeries referred to as revisions.
Per the Mayo Clinic, top surgery also carries the same risks as any other major surgery such as a bad reaction to anesthesia, excess blood loss, poor wound healing, and infections.
Finding a surgeon
Once you've decided that you want top surgery, it's time to find a surgeon to perform the procedure. Top surgery is done by plastic surgeons, and according to the American Society of Plastic Surgeons, you should be looking for one who is board certified, has previously performed the surgery in an accredited hospital or surgery center, and adheres to The World Professional Association for Transgender Health (WPATH) standards of care. The WPATH guidelines are the globally accepted standards for transgender healthcare.
In his comprehensive guide to finding the right top surgeon for you, trans activist, author, and speaker Finlay Games also emphasizes focusing on the surgeon's qualifications (via FinleyGames.com). Games adds that reputation within the trans community is important as well. If a top surgeon is good at their job, people will be sharing their experiences with that surgeon online. Another important tip from Games is to look at before and after photos posted on the surgeon's website or in online forums and look for bodies that resemble yours. This can give you a good idea of what surgery can and can't do for you.
Lastly, location is everything. If you have to travel to see the surgeon, costs can add up. You'll likely have several appointments before and after the surgery, and you'll likely have to travel to the surgeon each time. Be sure to consider this before scheduling a consultation.
Eligibility for top surgery
Unfortunately, wanting top surgery and finding a great surgeon isn't enough to get a procedure — or even a consultation — scheduled. Before you get in touch with your surgeon, you'll need to ensure that you meet their criteria. Each surgeon has their own set of eligibility standards, but most of them generally follow The World Professional Association for Transgender Health (WPATH) standards of care.
For top surgery, WPATH states that an eligible candidate must have a documented history of gender dysphoria, be able to provide informed consent to undergo the procedure, be in good mental health or have mental health conditions well-managed, and be of legal age to get top surgery. The age at which someone is legally allowed to undergo top surgery is determined by each state, and there is no universal standard. So, you'll need to check your state laws if you're under 18.
To prove a history of gender dysphoria, you'll need a letter from a mental health professional who's been working with you for a significant period of time. Taking hormones as part of your transition is not a prerequisite for top surgery, so if you haven't started, or don't want to, take testosterone, you're still eligible for top surgery.
BMI limits for top surgery
Some surgeons will not perform top surgery on people above a certain Body Mass Index (BMI). According to a paper published in the medical journal Transgender Health, medical professionals tend to associate higher body weight with health problems, specifically surgical complications (via National Library of Medicine). Because of this, many surgeons tell patients they'll need to lose weight to be eligible for top surgery.
However, the same paper, which reviewed the current medical literature on top surgeries performed on people with higher weights, found that BMI was not an indicator of poor top surgery outcomes. Another analysis of the current data published in the World Journal of Plastic Surgery similarly found that patients with higher BMIs did not have an increased number of complications compared to patients with lower BMIs (via National Library of Medicine). In fact, the rate of complications was nearly equal.
The researchers behind each of the papers also stated that denying patients top surgery based on their BMI had significant, negative impacts on mental health and quality of life. Both papers concluded that BMI should not be a factor in eligibility for top surgery and suggested that surgeons imposing BMI limits on the procedure reconsider their stance.
Luckily, there are several surgeons who don't impose BMI limits for top surgery. Transbmi.com is a resource put together by a fat trans person to help other fat trans folks find top surgeons who will perform the procedure on people of any body size.
Getting insurance to cover top surgery
These days, many insurance companies do cover gender-affirming surgeries, including top surgery, per the National Center for Transgender Equality. Unfortunately, they don't make it easy for you.
Nearly all insurance companies require a letter from a mental health professional stating that this surgery is medically necessary because of a diagnosis of gender dysphoria. Since this letter will likely be required by your surgeon as well, you've probably already got that letter, or it's in the works. The Transgender Legal Defense & Education Fund (TLDEF) has some helpful tips about the information that your mental health provider should put in that letter to ensure it includes everything your insurance company needs.
You'll also need to review your specific health insurance plan to determine the coverage rules. Sometimes information about trans healthcare won't be covered in your healthcare plan's regular service guide. Transcend Legal has a great video on YouTube about how to find the information you need. You'll likely need to speak directly to a customer service rep to ensure you understand the coverage.
Once you've thoroughly researched your insurance coverage, you'll probably need to get pre-authorized for the procedure. This process ensures that your insurance company will actually cover the costs related to top surgery when your medical team submits the bills. Even if your insurance company says it covers trans healthcare, receiving pre-authorization can be a complicated process. National Center for Transgender Equality has some great resources to help you through.
Top surgery costs
Top surgery can cost anywhere from $3,000 to $13,000 if you're paying the full cost without insurance, per TopSurgery.net. The amount varies widely by the surgeon, where they're located, and the surgical technique used. Additionally, there will be a separate bill for the anesthesiology and fees charged by the hospital or surgery center, which will add thousands of dollars to your total cost.
If your insurance company does cover top surgery, you'll still need to pay for a portion of the surgery, per the Transgender Legal Defense & Education Fund (TLDEF). Most insurance plans have a deductible that you need to meet before they'll cover any costs related to top surgery. Once your deductible is met, most insurance plans pay a portion of healthcare costs, called a co-insurance, until you've met an "out-of-pocket maximum." For an expensive procedure like top surgery, you might exceed both your deductible and out-of-pocket maximum amounts. Adding up your deductible and out-of-pocket maximum will give you a good idea of how much you'll be putting toward the overall bill. Note that all these costs will be higher if you choose an out-of-network surgeon.
On top of that, you'll need to factor in other costs such as transportation to and co-pays or bills for each appointment, multiple rounds of bloodwork, accommodations if you need to travel for surgery, and the things you'll need to buy for post-op recovery.
Making the most of your consultation appointment
Once you've found a surgeon who's a good fit, you'll have your first consultation appointment. As the folks at Stand With Trans point out, your consultation appointment is your chance to get all the information you need about preparing for top surgery, the procedure, and post-op recovery. It's essential to get all your questions answered at this appointment so you can play an active role in the decision-making process regarding your surgery, per Kaiser Permanente Medicine.
However, it can be difficult to remember what you want to ask the surgeon. Be sure to ask your surgeon which top surgery technique they believe is best for your body and why. Ask about their qualifications, how long they've been performing top surgery, and ask to see before and after photos of previous top surgeries they've done. Get information about preparing for top surgery like what lifestyle changes they recommend to make the surgery as safe as possible and what arrangements you'll need to make for your care post-op. Ask how long the surgery will take, whether it's inpatient or outpatient, and what the anesthesia process is like. Get information about recovery as well, like typical recovery times, when you'll be able to go back to work, and when you'll be able to do certain activities.
Bringing a list of questions with you is a great way to combat stress and anxiety and ensure you come out of your consultation with all the info you need.
Preparing for top surgery
Now it's time to actually start preparing for top surgery! Per Kaiser Permanente Medicine, there's a lot you need to do. And since preparing for surgery is ridiculously stressful, you'll need to find some time in there to take care of your mental health as well, as trans folks who've already had top surgery told Buzzfeed.
Even before you get your surgery date, start saving. You could put a portion of your paycheck into a special savings account or ask your family for cash instead of gifts around the holidays and your birthday. And remember to budget for the time you'll need to take off work. Depending on your job, your time off might be covered by FMLA or short-term disability. This will ensure that you get a portion of your paycheck during the time you're out. You'll need to work with your HR department or boss to fill out all the necessary paperwork as soon as you have your surgery date.
If you have any long-term issues like high blood pressure, start making adjustments to your diet and devise an exercise plan ASAP to get those under control. If you're a smoker, now's the time to quit. You'll be required to quit at least a month prior to surgery, but starting earlier is a good idea. To take care of your mental health, make sure you're reaching out to your pre- and post-surgery support team and getting to all your therapy appointments.
What to buy to make recovery easier
It's important to invest in some key items that will help make your recovery period easier, per Topsurgery.net. You'll need medical supplies. Gauze, medical tape, scissors, antibacterial ointment, and antibacterial soap will be essential for wound care, and polyurethane sheets as well as silicone gel and sheets are necessities for scar care. You'll also need a surgical binder, which the surgeon usually provides, but having one on hand just in case they don't is also a good idea.
As for medications, you'll want to stock up on Colace in case you're constipated after surgery, over-the-counter painkillers, and an antihistamine in case you have a reaction to the surgical binder. You'll also want to invest in some pillows to support your healing body since it'll be tough to get comfortable. A mastectomy pillow will protect your chest, a neck pillow can help you sleep upright, and some wedge pillows can be used for propping up your body in different positions.
You won't be allowed to shower for a bit after recovery, so you'll need some hygiene items as well. Body wipes and dry shampoo will be your go-to items for a while. Once you're cleared for a shower, a detachable showerhead and a bath sponge on a long handle will help a lot. Finally, since it will be hard to reach anything for a while, you might also want to invest in a back scratcher, a grabber tool, and a step stool.
What surgery day will be like
Knowing what happens when surgery day finally arrives can relieve some of the anxiety you may feel leading up to the momentous occasion. Stand With Trans suggests wearing loose-fitting elastic pants and a button-up or zip-up shirt because you won't be able to lift your arms after surgery, and bringing your own pillows to get as comfy as possible post-op.
In a Medium post about his top surgery, Grayson Bell, a trans author, shared that once you get to the hospital, you'll change out of your clothes into a hospital gown. A few nurses will prep you for surgery. They'll be asking questions, drawing blood for pre-surgery tests, and placing an I.V. to administer fluids and medicine before, during, and after surgery. At some point before, the anesthesiologist will come to talk to you about your medical history, explain the process, and have you sign a consent form for the anesthesia.
According to Johns Hopkins Medicine, your surgeon will drop by before the surgery to draw on your chest, marking where they'll be cutting. They do this while you're sitting up to ensure that the results will look natural. You'll then be wheeled into the operating room and moved to a surgical table. The anesthesiologist will put an oxygen mask on you to administer the anesthesia, then you'll drift off to sleep. Top surgeries typically take three to four hours and are usually outpatient procedures, meaning you'll head home the same day.
What recovery from top surgery is really like
When you wake up in the recovery room, as Grayson Bell shared on Medium, you may be completely out of it, or you could be totally alert. It depends on your individual reaction to the surgical drugs.
After some time, you'll be able to eat. In a Medium post about their top surgery, Oak, a writer for Psychology Today, shared that some hospitals have anti-nausea popsicles that will help settle your stomach and soothe your throat, which will be sore from the tube the doctors put in during surgery. Once you eat and urinate, you'll be sent home with detailed post-op instructions.
You'll be incredibly sore and won't be able to do much for a while. In a blog post, Christopher Inglefield shared that recovery was way more difficult than he imagined, and he needed a lot more help than he expected (via The London Transgender Clinic). Bell and Oak had similar experiences. They all wrote that they were tired all the time, and needed a lot of rest and around-the-clock care. You won't be able to lift your arms above shoulder level or lift anything more than five pounds. Getting up and down from a seated or lying down position will also be difficult because you can't push yourself up.
Some people also get really emotional and even depressed post-op. This is normal, and be sure to get support from loved ones and/or a therapist if it happens to you.
Caring for yourself after top surgery
Recovery from top surgery is definitely a marathon, and it feels just as difficult. Per the Gender Confirmation Center, for the first few days, you'll need someone to help you with pretty much everything. Micah, a trans writer who runs the blog genderqueer.me, suggests sleeping as much as possible on a recliner or in bed with a "pillow fort" so you can get as comfortable as possible.
For the first week or so, you'll have two tubes coming out of your chest attached to bags that collect blood from your incisions. You'll need to empty the bags and record how much fluid they collected multiple times a day. You'll also have bandages on, which you shouldn't remove. Keep them clean and dry. About a week after surgery the drains will be removed. Then you'll be able to shower normally. You'll still have to wear a compression garment or ace bandages around your chest even after the dressings are removed to reduce swelling.
A week post-surgery you might feel up for some light activity, but don't overdo it. It's important to understand that it will take at least a couple of weeks to feel semi-normal again, at least six weeks before you're back to your regular activity level, and up to six months to fully recover from top surgery. Eating well, doing some gentle movement, and leaning on your friends and family will help make recovery easier, but it's a long road.
Life after top surgery
Getting to and through the top surgery procedure and recovery may seem excruciating, but the payoff is absolutely worth it. In an essay about his top surgery for The Guardian, Freddy McConnell, a trans journalist, wrote about the pure joy of seeing his chest for the first time a week after surgery. He described it as seeing his true self in the mirror for the first time.
Xander Perez, a trans man who wrote about his top surgery for Jefferson Health, had a similar experience. He recounted how he cried tears of joy nearly every time he looked in the mirror, and what it was like to be truly perceived as a man by new acquaintances post-surgery.
Both men wrote about the delight of presenting the way they wanted to for the first time. Perez wrote that his favorite shirts fit him better than ever and described the feeling of not having to hide his chest. McConnell, who was only two months post-op when he wrote the essay, shared his excitement for going shirtless for the first time since before puberty during the upcoming summer months.
Perez and McConnell's joy post-top surgery isn't unique. A study published in the Journal of the American Medical Association found that top surgery was associated with major mental health improvements (per Jama Network). For the majority of trans men and masculine non-binary or gender non-conforming folks, life after top surgery is the life they've always wanted to live.