Sleep Apnea: How The Disorder Affects Your Skin (& Other Symptoms You Should Know)
The relationship between skin and sleep is often underestimated. Sure, you've probably heard that a good night's sleep is essential for various reasons, but why is this the case? For one, during sleep, our skin undergoes a process of repair and regeneration, and lack of sleep or poor quality sleep can negatively affect the skin.
Sleep apnea is a common sleep disorder potentially affecting billions of folks, and it can lead to poor sleep quality and sleep deprivation (via Lancet Respiratory Medicine). What's more, it has been linked to various health problems, including cardiovascular disease, diabetes, and mental health. However, it can also impact skin health, like any other sleeping condition.
As a 2019 study in the Journal of Clinical and Aesthetic Dermatology highlights, a growing body of scientific evidence correlates disruptions in our circadian rhythm with skin health. For the uninitiated, our circadian rhythm plays a huge role in regulating various bodily functions. It is essentially an internal clock controlled by our brain. It uses light to trigger crucial activities such as DNA repair while we sleep. This is also why disruption to this rhythm, like sleep apnea, can be so damaging, as it limits our bodies from carrying out these essential functions. Here, we delve into what these functions are, how they affect the skin, and other ways sleep apnea can impact our overall health.
What is sleep apnea?
According to the National Heart, Lung, and Blood Institute, sleep apnea is a common sleep disorder characterized by repeated breathing pauses and restarts during sleep, which can cause a decrease in oxygen levels in the body. The two types of sleep apnea are obstructive sleep apnea and central sleep apnea. Obstructive sleep apnea occurs when the upper airway becomes blocked during sleep, while central sleep apnea happens when the brain fails to send the proper signals to control breathing. Given the nature of sleep apnea, it should be no surprise that it has such a detrimental effect on our bodies.
To explain, Harvard Medical School measured the average amount of oxygen in a person's blood with and without sleep apnea. In particular, researchers looked at blood oxygen levels or oxygen saturation measurements. Oxygen saturation represents the percentage of oxygen-carrying hemoglobin in the blood bound to oxygen molecules.
They found that while without any obstructions, a person will have a blood oxygen level of roughly 96% to 97%, those with sleep apnea only have 80% to 89% oxygen saturation or sometimes even less. Although this might not seem like much of a difference, our body relies on consistent oxygen levels to function properly. And with sleep apnea, the effect of low blood oxygen can cause a variety of symptoms and issues.
What are the typical symptoms of sleep apnea?
Sleep apnea affects people in a variety of ways, including everything from mild disturbances to serious conditions that you should be aware of. Those with sleep apnea often experience frequent loud snoring and gasping for air during sleep. They may also find themselves with a dry mouth or headaches, sexual dysfunction or decreased libido, and waking up often to urinate at night. The Sleep Foundation also notes that due to the nighttime disturbances that sleep apnea causes, many people often see symptoms roll over into waking hours with issues such as daytime tiredness that can lead to problems in learning, focusing, and reacting. Several notable severe conditions may also arise as complications of sleep apnea.
Sleep apnea has been associated with many forms of cardiovascular disease, including hypertension, stroke, and heart failure. According to a study in the Journal of the American Heart Association, adults with sleep apnea not only have an increased risk of developing cardiovascular disease but also have worse outcomes if they suffer from sleep apnea already.
Another prevalent condition is type 2 diabetes. Research in the Journal of Diabetes Investigation suggests that sleep apnea patients are more likely than those without to develop type 2 diabetes, while more than half of type 2 diabetes patients suffer from sleep apnea already.
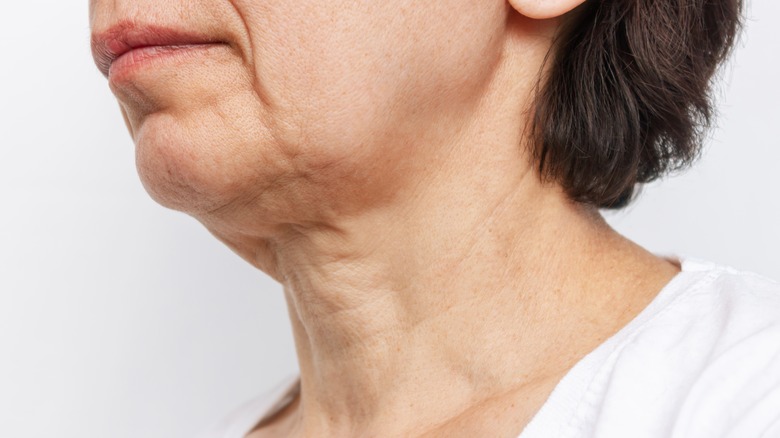
How sleep apnea affects aging
Often, people with sleep apnea do sleep through the night, so they may not recognize the effect it has on their sleep and, by extension, their skin. Humans have two major sleep stages: light and deep sleep. Although deep sleep makes up a smaller fraction of the sleep stages you go through at night, it is one of the most vital for cognitive processes and biological renewal.
However, research in the Journal of Basic and Clinical Neuroscience uncovered that people with sleep apnea may get more light sleep but do not benefit from as much deep sleep as those without. This aspect of sleep apnea means that overall the integrity of bodily functions gets impaired. For skin, these functions include how well the skin's barrier can protect against external factors, such as UV light, pollution, and weathering, among others.
As such, a study in the Journal of Clinical and Experimental Dermatology suggests that a lack of sleep can accelerate skin aging. Namely, they highlight lack of sleep can compromise skin barrier function, making the skin more susceptible to damage and dehydration. Unfortunately, skin proteins such as collagen rely on water to perform, meaning they lose structural integrity, an important aspect of preventing wrinkling.
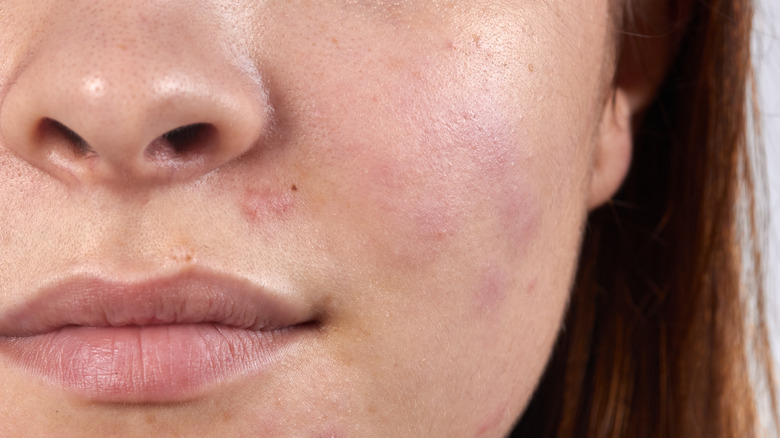
Does sleep apnea cause acne?
In short, yes, sleep apnea does affect the development of acne in several ways. For instance, a study from the Indian Journal of Dermatology, Venereology, and Leprology explores the relationship between sleep quality and facial sebum levels in women with acne vulgaris. The study found that poor sleep quality was associated with increased sebum production, contributing to acne development.
However, in the Journal of Clocks & Sleep (MDPI), researchers assert that there was only a limited connection between sleep quality and acne. They instead posit that acne is more likely to be induced by depressive symptoms or poor life quality. Interestingly, these findings correlate with other research, suggesting a relationship between sleep apnea and hormonal imbalance, which is associated with acne.
What's more, a study in the Archives of Medical Science Journal looks at sleep apnea and disruptions in the body's hormonal regulation, particularly concerning cortisol. This hormone regulates inflammation and stress. The study authors measured cortisol, insulin, and sex hormones before and after sleep apnea treatment. Since those without treatment had higher levels of all these hormones, the results suggest that hormonal imbalances caused by sleep apnea could contribute to the development of acne.
The relationship between pigmentation, Sun damage, and sleep apnea
According to the National Cancer Institute, hyperpigmentation is a normal and benign condition. It occurs due to the excessive production of melanin, the pigment responsible for giving color to our skin, hair, and eyes. This can happen for various reasons, but you will often see the main factors cited as sun exposure, hormonal changes, and inflammation.
These factors influence the resulting types of hyperpigmentation you may have, such as melasma, age spots, and post-inflammatory hyperpigmentation (PIH), which happens after an injury. In fact, a survey in the International Journal of Women's Dermatology found that melasma and PIH were among the most common types of hyperpigmentation. However, while these skin conditions may be prevalent, certain factors can increase your susceptibility, and sleep apnea is one of them.
For instance, melasma research in the Journal of Clinical and Aesthetic Dermatology suggests that UV exposure coupled with poor sleep quality can cause inflammation in the skin, which can trigger the production and release of melanin pigments and inflammatory cytokines (proteins responsible for cell growth) that contribute to the development of melasma, as well as other forms of hyperpigmentation and skin issues
Other influences of sleep apnea on inflammation and skin conditions
Delving deeper into the inflammation process and how it affects the skin, we can see quite clearly why sleep apnea may be the source of many skin conditions. In an article published in the Journal of Current Sleep Medicine Reports, reviewers identified how sleep apnea affects several skin conditions, such as psoriasis, atopic dermatitis, and basal cell carcinoma (skin cancer).
Starting with psoriasis, a chronic inflammatory skin condition characterized by red, scaly patches of skin, the study suggests that sleep disturbance from sleep apnea can exacerbate this condition by inducing an inflammatory response in the body. Another inflammatory issue is atopic dermatitis – also known as eczema, a common skin condition that causes dry, itchy, and inflamed skin. The study found that those with sleep apnea were 1.5 times more likely to develop atopic dermatitis.
Lastly, and perhaps the most troubling, is skin cancer. The study suggests that skin cancers may be associated with sleep apnea due to the body sending signals to create new blood vessels inappropriately in response to low blood oxygen, which can contribute to the growth of cancer cells. While more research is needed to fully understand the relationship between sleep apnea and skin conditions, the findings do suggest an adverse link between them.
Can sleep apnea cause redness?
To know whether sleep apnea could cause skin redness, it's essential to understand the underlying conditions that might be responsible. According to the American Academy of Dermatology, the top six most common causes include acne, sunburn, hot flashes, seborrheic dermatitis, rosacea, and allergic reactions.
Since we have already touched on the relationship between sleep apnea and acne, sun exposure, and hormonal imbalance, we'll focus on the last three. Both seborrheic dermatitis and rosacea are forms of eczema, per the National Eczema Association. Whereas seborrheic dermatitis is again the result of inflammation which we've seen is closely linked to sleep apnea, the case of rosacea is slightly more complex.
As described by the National Rosacea Society, rosacea can be caused by a combination of issues, from misfires in the brain to microscopic insects. Interestingly, however, research suggests a correlation between poor sleep and the condition. Research in a recent edition of the Journal of Cosmetic Dermatology proposes that rosacea is a systemic disease, meaning that it results from a whole-body disorder rather than being contained to just the skin. As such, sleep, which is intrinsically a body-wide phenomenon, might be the key to understanding it, specifically why disruptions like sleep apnea could trigger rosacea.
Why does sleep apnea affect skin?
Based on what we've covered so far, there are a few different theories behind why sleep apnea affects the skin. Referring to research published in the Journal of Current Sleep Medicine Reports, we can summarize that the central pathways that sleep apnea affects skin are hypoxia, inflammation, and vascularization. Hypoxia is a lack of oxygen in the body. This happens when the upper airway becomes blocked, and the individual briefly stops breathing. As a result, the oxygen level in the body decreases, leading to hypoxia. This lack of oxygen can cause skin cells to become stressed, inducing cellular damage, which can cause premature aging, dullness, and even skin diseases.
As discussed, sleep apnea can also cause inflammation in the body. This happens when the body's immune system tries to fight off infection or injury. Inflammation can cause the skin to become red, swollen, and painful. Over time, chronic inflammation can lead to the breakdown of collagen and elastin, which are essential for healthy skin. This can cause premature aging, wrinkles, and sagging skin.
There is also a risk of vascularization as sleep apnea can cause changes in the blood vessels in the body, leading to the formation of new blood vessels. This can cause skin problems such as redness, visible blood vessels, and potentially skin cancer. While some of these issues are specific to sleep apnea, much of the damage comes directly from sleep's role in maintaining our bodies.
Why is sleep so important for skin?
Simply put, sleep is an essential aspect of our daily lives and profoundly impacts our overall health and well-being. In particular, as an issue in the Medical Hypotheses Journal explains, disrupted sleep patterns can lead to decreased skin barrier function, increasing the risk of skin dryness, irritation, and inflammation. Sleep deprivation can also result in decreased collagen production, a vital protein that keeps skin firm and elastic when our skin barrier is impaired. We can summarize these effects in three ways: Dehydration, hormone imbalance, and stress.
Sleep deprivation can compromise the skin barrier, causing dehydration and limiting its effectiveness at protecting against external factors such as pollution and bacteria. This results in a damaged skin barrier leading to the skin issues we described above. Similarly, a lack of sleep can also factor in developing stress or low mood. Stress and low mood can cause the body to produce more cortisol, leading to inflammation and the breakdown of collagen and elastin, resulting in premature aging and sagging skin.
We also see that poor sleep quality can cause hormonal imbalances in the body. Specifically, it can decrease growth hormone levels, which is essential for repairing and regenerating skin cells. This hormonal imbalance can lead to skin problems such as hormonal acne, dryness, and wrinkles.
How to repair skin damaged by sleep apnea?
To treat the skin issues that sleep apnea causes, it may be best to approach it from two fronts. That is to say, if you only treat the skin, conditions may reoccur if the body itself is not also treated. As such, we recommend looking at both the cause and symptoms of sleep apnea-induced skin problems. Starting with treating apnea, we'll refer to work in the Kaohsiung Journal of Medical Sciences, which reviews the latest treatments.
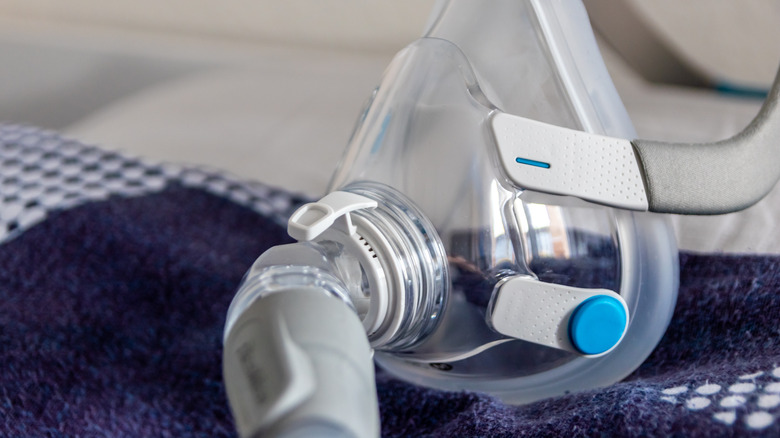
Continuous positive nasal pressure (CPAP) is typically the first line of defense for treating sleep apnea. CPAP involves wearing a mask over your nose and/or mouth while you sleep, connected to a machine that delivers a steady stream of air pressure to keep your airway open and prevent it from collapsing during sleep. The air pressure acts like a splint, keeping the airway open and allowing air to flow into the lungs normally. This helps to reduce or eliminate sleep apnea symptoms such as snoring, gasping, and pauses in breathing.
However, alternative treatments, such as oral appliances or mini-implants, are available for patients who cannot tolerate CPAP. Other treatments include avoiding alcohol and sedatives, avoiding lying on the back during sleep, and weight loss. Patients must work with a healthcare provider to determine the best treatment approach based on individual needs and medical history.
Treating the skin
Once the underlying cause is dealt with, treating skin issues can be done according to your condition or problem. Now, let's talk about aging, acne, and skin barrier-related issues.
Before you use retinol, you should know that retinoids are vitamin A derivatives that can increase collagen production and improve the appearance of fine lines and wrinkles. Research in the Journal of Dermato-Endocrinology notes that retinoids are among the most effective treatments for aging skin but can also cause skin irritation, redness, and sensitivity (though this is usually temporary). Another effective treatment that works towards restoring the skin barrier is topical antioxidants. These substances protect the skin from damage by neutralizing free radicals, which can damage cells. These antioxidants, such as vitamins C and E and green tea extract, have been shown to improve and brighten the skin, reduce redness, and minimize fine lines.
For more severe skin issues, they recommend treatments such as laser resurfacing and chemical peels for acne. Chemical peels are treatments that use acids to remove the outer layers of the skin, which can improve skin texture appearance. In contrast, laser resurfacing is a treatment that uses lasers to remove the outer layers of the skin, which can improve fine lines and wrinkles. In both cases, the article notes that treatments must be performed by a qualified professional and that patients may experience temporary redness, swelling, and sensitivity after.
Differences between men and women
Lastly, while we have been looking at the effects of sleep apnea on skin exclusively, it is important to note that the condition can affect men and women differently. The differences between men and women with sleep apnea can be wide-ranging from sleep quality, number of episodes, and even severity.
Moreover, according to research in the Journal of Sleep Medicine Reviews, the pathology — that is, the likely cause for the disease — can differ substantially as well. For instance, sleep apnea affects genders differently due to factors such as upper airway anatomy, neurochemical mechanisms, and sex hormones. Despite this, researchers and clinicians tend to group both genders together in scientific investigations and clinical trials. However, it may be beneficial to study how the genders respond to different treatments or if alternative gender-specific therapies can be pursued.
We also see the researchers found differences in sleep apnea symptoms, which may lead to under-reporting or misdiagnosis. Though sleep apnea is more common in men than women, women often present other symptoms, such as insomnia and depression, giving rise to underdiagnosis and increased risk for health problems. This may be because the male-to-female ratio is higher for severe cases of sleep apnea, which may contribute to the higher number of men in sleep clinics. For these reasons, it is so important to understand gender differences in sleep apnea so that clinicians can improve diagnosis, treatment, and outcomes.